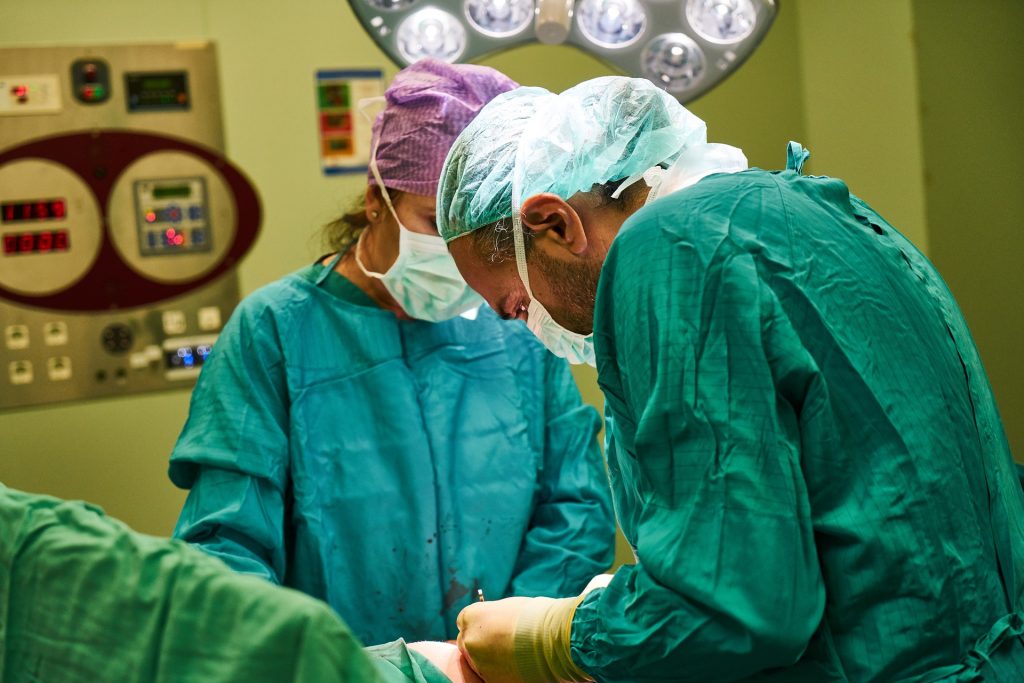
£10bn could be the price for buying operations in the private sector over the next four years to treat patients that the NHS does not have the capacity to treat, according to a newly published contract notice published by NHS England, but will it become a longterm arrangement?
Millions of patients had their treatment put on hold whilst the NHS battled Covid-19 and waited with considerable anxiety not knowing when their turn would come. They deserve urgent care and if using beds and theatres in private hospitals is the way to guarantee it, then it should be done, but the unremitting desire of governments to outsource and the long record of failures rightly sets off alarms.
The deal should be a time-limited arrangement and certainly not a replacement for the core requirement for a credible new plan to lift NHS capacity. For a decade the government has ignored the evidence about the levels of resources and staffing needed to match the rising health needs of our community and have run-down key services like public health, hitting the poorest worst. No more. This new funded plan must start now and run in parallel with any deal done with the private sector.
Bed numbers had been cut steadily for over a decade and before Covid there was a staffing crisis with over 100,000 vacancies, including 40,000 nurses. For the first time on record, in late 2019, the NHS was missing all its targets, including A&E waiting times, cancer treatment and non-urgent surgery. The waiting list for non-urgent procedures was at 4.4 million, also at a record level.
The NHS needs more than private-sector help, but even if the deal is done will they deliver? The public may rightly question the motives of private companies – that have been positioning themselves to profit from the NHS for years. Outsourcing in the NHS has delivered a catalogue of failures and examples of companies gaming the system and providing poor value.
Successive governments have made it a pivotal aim to encourage greater for-profit involvement, despite the stack of problems. So forgive the cynics who perceive a glint of opportunism in ministers’ eyes at this new deal.
A lifeline for companies
For the private health providers, the NHS deal has been a lifeline, giving them a guaranteed income stream in very difficult times. These companies already rely heavily on work from the NHS – at over 80% of Ramsay’s income and around 40% of BMI/Circle and Spire’s income – and this was falling prior to the pandemic as the NHS was instructed to reduce the use of the private sector to save money.
With the lockdown came a cessation of all private work – without the March deal from the government the companies would have found it very difficult to survive. Although they have now been allowed to restart some private work, worldwide recession beckons, and so making the NHS deal will be an even more important part of their strategy.
Make no mistake, the public should have the upper hand in this negotiation, as many private health companies have suffered flagging fortunes of late and are already being propped up with by £400m a month in public tax receipts, so the government should dominate the terms to make this agreement work for patients and the NHS.
Paying for treatments not delivered
We should learn too from earlier efforts to dragoon the private sector in to help with waiting lists prior to 2010, which whilst contributing to reducing the delays for some patients, resulted in over £200m in payments to providers for treatments that didn’t take place.
Don’t forget the position of staff, who need continual training, a cost largely born by the NHS. Shouldn’t then the NHS be compensated by the private companies who lure staff away? Improved NHS pay and working conditions are a top priority and would help to reward and keep precious NHS staff.
What about the current NHS Plan? Whatever your view it has not yet delivered a credible strategy to: recruit and retain its workforce, to build and repair NHS facilities both in the acute and community sectors, to set proper funding, end creeping privatization and put in place accountable structures so that the NHS can be properly planned and run in the public interest. The NHS and its patients deserve better.
Ten Questions about the deal:
Will the government publish details of the contracts with the private hospitals and allow Parliament to scrutinise them? Commercial confidentially is traditionally cited to keep these deals out of the public view but in March the government also suspended the normal requirement to advertise and award contracts through open competition, so even a partial view has been obscured.
Will the government ensure that a plan to raise NHS capacity runs in parallel with any deal so that the NHS can take over all work as quickly as possible? NHS beds numbers have been cut in recent years despite rising demand. There is a £6bn backlog in building repairs and a shortfall of at least 100,000 staff and yet there is no credible plan to fund an expansion of services.
How long will this arrangement stand? The Cameron government oversaw a vast experiment with private sector involvement in the NHS. Seven years later NHS England called for a new law to remove the compulsory tendering of NHS contracts, but no change has happened. NHS expenditure on the private sector still grows and with some concern that without controls the government could exploit this opportunity to expand the role of the private sector.
Will the private sector receive the NHS rate in payment and how will the government prevent the waste that has happened in the past? The NHS tariff sets out the price at which NHS hospitals receive payment, the private sector should not receive more.
There is a precedent for badly made large-scale deals between the NHS and private hospitals – the contracts for the Independent Sector Treatment Centres (ISTC), which were begun with the aim of reducing the waiting lists back in 2003 to 2007 were later found to have wasted taxpayer money to the tune of almost £500 million including a series of ‘needless’ payments written into contracts that were virtually risk-free for the private companies involved.
How will safety measures in the NHS be applied and checked across private sector sites? A report in 2018 by the Centre for Health and the Public Interest identifies what they believe is a systemic patient safety risk within private hospitals.
They identify that post-operative care in most private hospitals is carried out by an inexperienced junior doctor, most units lack intensive care facilities and the consultant who carries out the surgery is permitted to be off-site, in some cases 45 minutes away CHPI also contends that the data on patient safety incidents in private hospitals is poor and private hospitals are not required to notify patient safety incidents in the same way as the NHS.
Will the cost of staff training, normally borne by the NHS be reflected in the terms of the agreement? The BMA says the NHS Standard Contract should include a clause requiring independent sector providers to contribute towards the education and training of the NHS workforce. In UK the private sector makes use of staff who have been trained in the public sector but makes a negligible contribution to training costs.
How will the government make sure the financial viability of NHS is not affected? NHS hospitals rely on income from treating patients to sustain their activities. It is therefore essential for their sustainability for the arrangement with the private sector to be time-limited.
Who will control the allocations and ensure the best clinical decisions? In the past, contracted companies have falsified performance data and there have been accusations that caseloads are manipulated to reduce their costs and operations carried out needlessly
What happens to patients on the waiting lists in areas where this extra capacity is not available? The additional capacity will not always be where the longest waits exist. There is already inequity in the provision, how will this be managed?
Can the government guarantee transparency over the operation of this deal? How will the contracts be monitored and information published given the lack of resources traditionally spent on this aspect and the fact that the Freedom of Information Act does not apply to private providers?
Despite the situation the NHS finds itself in, there should be no reason that any deal with the private sector should not be fully scrutinised.
Without adequate scrutiny of the deal, the NHS could simply end up bailing out an ailing private sector – to the tune of billions of pounds.
The evidence so far of the use of the private sector over the past three months shows that the private sector’s help for the NHS has been limited, but in exchange, it has received millions to pay its debts and operating costs.
Dear Reader,
If you like our content please support our campaigning journalism to protect health care for all.
Our goal is to inform people, hold our politicians to account and help to build change through evidence based ideas.
Everyone should have access to comprehensive healthcare, but our NHS needs support. You can help us to continue to counter bad policy, battle neglect of the NHS and correct dangerous mis-infomation.
Supporters of the NHS are crucial in sustaining our health service and with your help we will be able to engage more people in securing its future.
Please donate to help support our campaigning NHS research and journalism.